Stress does more than affect your mood, it can influence metabolism and overall metabolic health. When stress becomes chronic, the body’s stress-response system may remain activated, increasing cortisol exposure and altering appetite, cravings, fat storage, and blood sugar control. Over time, this can make weight management more challenging, especially around the abdomen. This article explores the hormonal connection between stress and weight gain, and how supportive, realistic strategies can help protect long-term hormone balance.
Stress is often treated as an emotional experience, but it is also a deeply biological one. When stress becomes chronic, it can influence how the body regulates appetite, stores fat, and uses energy. This is one reason why weight changes during stressful periods are not simply about willpower or discipline, they are often rooted in physiology.
At the center of this response is cortisol, one of the body’s primary stress hormones. Cortisol is essential for survival and plays an important role in blood sugar control, energy regulation, and the body’s ability to respond to challenges. But when stress becomes persistent, repeated cortisol exposure may begin to affect metabolism in ways that make weight gain, especially abdominal weight gain, more likely.
Understanding this connection can help shift the conversation around weight from blame to biology.
The HPA Axis: The Body’s Stress Command Center
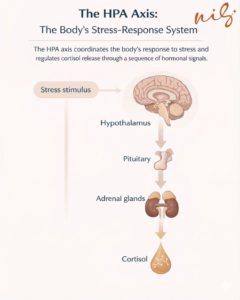
When the brain perceives stress, whether physical, emotional, or psychological—it activates the hypothalamic-pituitary-adrenal (HPA) axis, the body’s central stress-response system.
This happens in a sequence:
• The hypothalamus signals that the body is under stress
• The pituitary gland relays that message
• The adrenal glands respond by releasing cortisol
In the short term, this response is protective. It helps increase alertness, mobilize glucose for quick energy, and prepare the body to handle immediate demands.
The problem begins when stress is no longer occasional. With chronic stress, the HPA axis may remain repeatedly activated, keeping cortisol levels elevated or dysregulated over time. This can begin to influence appetite, cravings, insulin resistance, sleep quality, recovery, and fat storage.
In simple terms: the body stays in a state of “energy protection,” even when there is no immediate threat.
How chronic stress triggers weight gain: the cortisol connection
Chronic stress does not automatically cause weight gain, but it can create conditions that make weight regulation harder, especially in women navigating PCOS weight loss, thyroid shifts, or early metabolic changes.
Cortisol is involved in:
• Blood glucose regulation
• Appetite signaling
• Fat distribution
• Energy mobilization
• Interaction with insulin and other metabolic hormones
Over time, prolonged cortisol exposure may:
• Increase appetite, especially for highly palatable foods
• Intensify cravings for sugar- and fat-rich foods
• Disrupt insulin sensitivity
• Shift fat storage toward the abdominal region
• Make recovery and body composition goals harder to maintain
This helps explain why many people notice that during high-stress periods, they may feel hungrier, snack more, crave comfort foods, or gain weight around the midsection despite trying to stay “on track.”
Stress, cravings, and why willpower is not the problem
One of the most important links between stress and weight gain is reward-driven eating.
Under chronic stress, the brain becomes more likely to seek quick comfort and reward. Cortisol can interact with appetite signals and the brain’s reward pathways, increasing the appeal of foods that are high in sugar, fat, or salt.
This does not mean stress always leads to overeating, but it can make it harder to feel satisfied and easier to reach for “quick relief” foods, especially when combined with fatigue, poor sleep, or mental overload.
That is why stress-related eating often feels less like hunger and more like:
• Craving
• Urgency
• Emotional relief
• Loss of control around specific foods
This is not a lack of discipline. It is often a stress-adapted behavior.
Cortisol influences how and where fat is stored. Higher long-term cortisol exposure has been linked to a greater tendency toward visceral fat accumulation.
The science of cortisol belly fat: why stress causes abdominal weight gain
One of the most common patterns seen under chronic stress is central or abdominal weight gain.
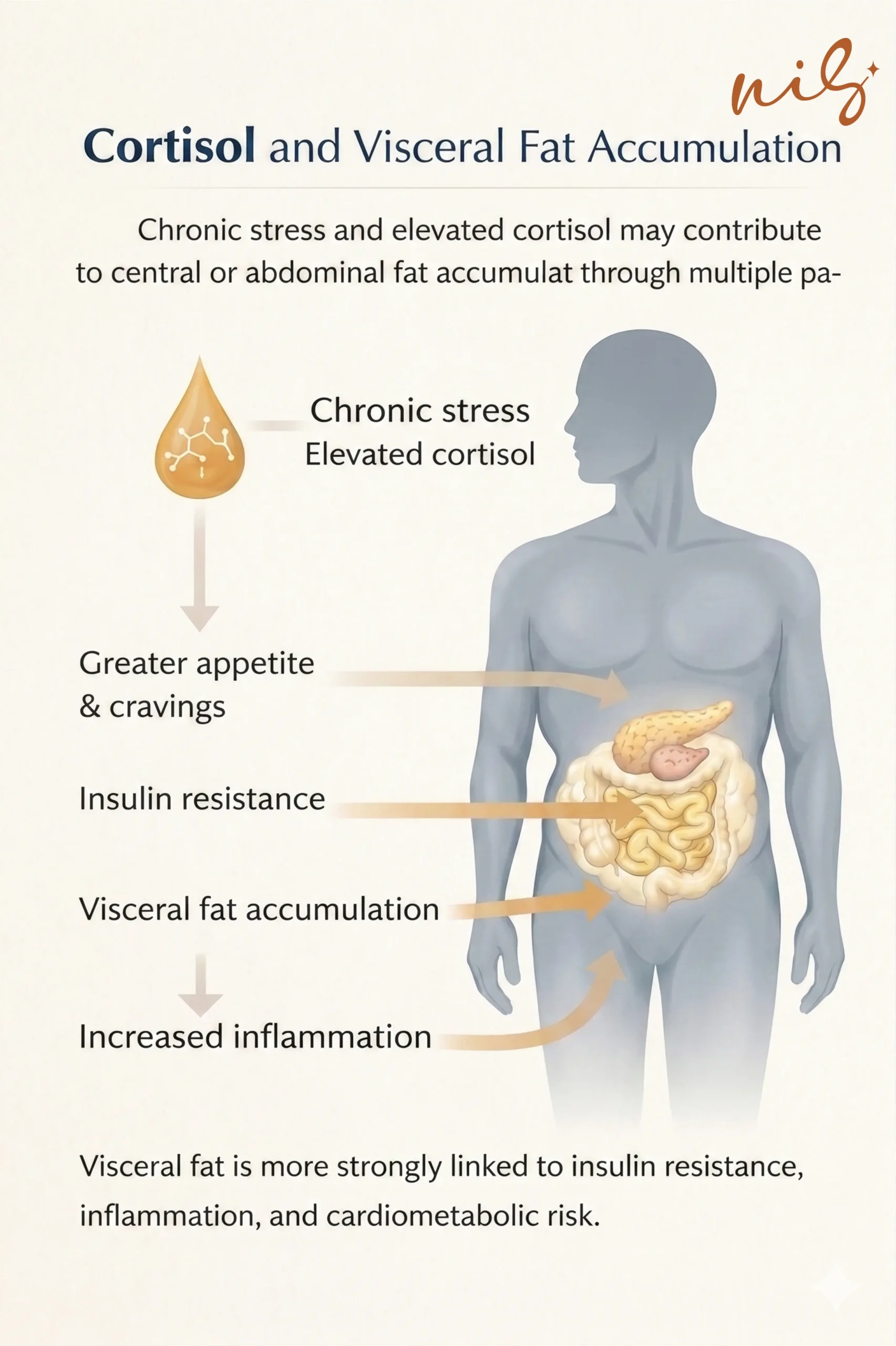
This is partly because cortisol influences how and where fat is stored. Higher long-term cortisol exposure has been linked to a greater tendency toward visceral fat accumulation.
Visceral fat is metabolically active and more strongly associated with:
• Insulin resistance
• Inflammation
• Cardiometabolic risk
At the same time, chronic stress can indirectly worsen this pattern by:
• Disrupting sleep
• Increasing cravings
• Reducing movement
• Increasing inflammation
• Affecting blood sugar regulation
This is also where digestive health and the gut microbiome can begin to shift under stress, further influencing how the body processes food and stores energy.
How stress disrupts sleep, hormones, and metabolic health in women
It is important to keep this balanced: cortisol is not the sole reason people gain weight.
Weight regulation is influenced by many factors, including:
• Sleep
• Nutrition
• Physical activity
• Insulin sensitivity
• Hormonal health
• Thyroid health
• Emotional wellbeing
• Chronic stress load
For some women, especially during phases like perimenopause symptoms, stress can amplify existing hormonal shifts rather than act alone.
What actually helps: nutrition and lifestyle strategies to lower cortisol
If stress is part of the picture, the answer is not more restriction or punishing exercise.
A more supportive approach includes:
• Regular, balanced meals to support blood sugar control
• Adequate protein and fiber for satiety
• Resistance training and walking
• Consistent sleep to regulate cortisol rhythm
• Stress management practices
• Realistic calorie deficits
If stress is also showing up as bloating, irregular digestion, or discomfort after meals, supporting the gut alongside the nervous system can make this process feel much easier, this is where a structured approach like a gentle gut reset can help restore balance.

Stress is not just something we feel, it is something the body processes hormonally. When stress becomes chronic, repeated cortisol exposure can influence appetite, cravings, fat storage, and metabolic balance.
That does not mean cortisol is the enemy. It means the body is trying to adapt.
Weight gain under stress is not always a sign of poor discipline. Sometimes, it is a sign that the nervous system has been under pressure for too long.
Supporting metabolic health means looking beyond calories alone. It means making space for recovery, regulation, and habits that work with the body, not against it.
And when stress, hormones, and metabolism start to overlap in more complex ways, having the right guidance can help you understand your body more clearly and work with it, not against it, something we focus on deeply inside the ONE Program at Nutrition in Sync, where the goal is not just weight loss, but restoring balance at the root.


